
Healthy Gut
The digestive system is the long tube that extends from the mouth to the anus. The gut is a casual term that usually refers to the stomach, small intestine, and large intestine.
This article describes the functions of a healthy gut and factors that contribute to its health or damage.
The gut has 3 important roles:
1. Digesting and Absorbing Nutrients
Your cells need nutrients from food to function properly. The gut is where digestion and absorption happen. If your gut is inflamed, the cells that line the stomach and the small intestine will not produce enough enzymes to break down food particles properly. Even with the presence of enzymes from the pancreas, an inflamed gut won’t absorb nutrients properly. This can lead to nutrient deficiencies, gas, bloating, and constipation.
You are NOT what you eat. You are what you DIGEST and ABSORB
Your body sloughs off old intestinal cells and replaces them with new cells every 2 to 4 days. For new cells to develop and proliferate properly, nutrients like B vitamins (folate and vitamin B12), vitamin A, vitamin C, zinc, amino acids, fatty acids, and butyric acid (short-chain fatty acid, more on that below) are needed. Without them, the new cells won’t function properly, produce even fewer enzymes, and lead to more nutrients deficiencies.
2. Hosting the Microbiota (also called the gut flora)
Believe it or not, there are 10 times more bacteria in your gut than human cells in your entire body. More than 400 different species have been identified and we will learn about more in the future. Healthy gut microbes live in a symbiotic relationship with us, the hosts! Conditions like heart disease, diabetes, and obesity have been recently linked to a having unhealthy balance in gut bacteria.
Healthy gut flora performs several jobs in our gut. Some bacteria manufacture vitamins like vitamin K2, vitamin B12, B6, B5, folate, and biotin. They digest fiber from food (we don’t have the enzymes to break down fibers) and produce short chain fatty acids, which nourish the cells of the intestinal lining. Healthy bacteria protect us by fighting pathogenic bacteria, yeast, and parasites.
Estrogen dominance is a common phenomena in women of all ages, resulting in hormone imbalances, weight gain, bloating, swelling, mood swings, heavy or irregular periods, and headaches before cycles. Healthy gut bacteria restore hormone balance because they break down excess estrogen so it can be excreted outside of the body. Without healthy bacteria, estrogen gets reabsorbed into the body and is deposited in the breast, uterus, and ovaries, worsening the symptoms and potentially leading to fibroids, tumors, PMS, and others.
3. Protection from Foreign Invaders
Your gut is just like your skin, but from the inside. If you think about it, the content of your digestive tract is OUTSIDE and your blood, organs, cells, etc are on another side, INSIDE. Food, chemicals, water, toxins, microbes, and medications have to pass through the lining of the gut to reach your cells.
Think of your gut lining as a window screen that prevents bugs from coming inside your home. A healthy gut protects you from foreign substances like bacteria, toxins, and undigested foods and will only allow completely digested micronutrients, vitamins, minerals, antioxidants, and water to be absorbed.
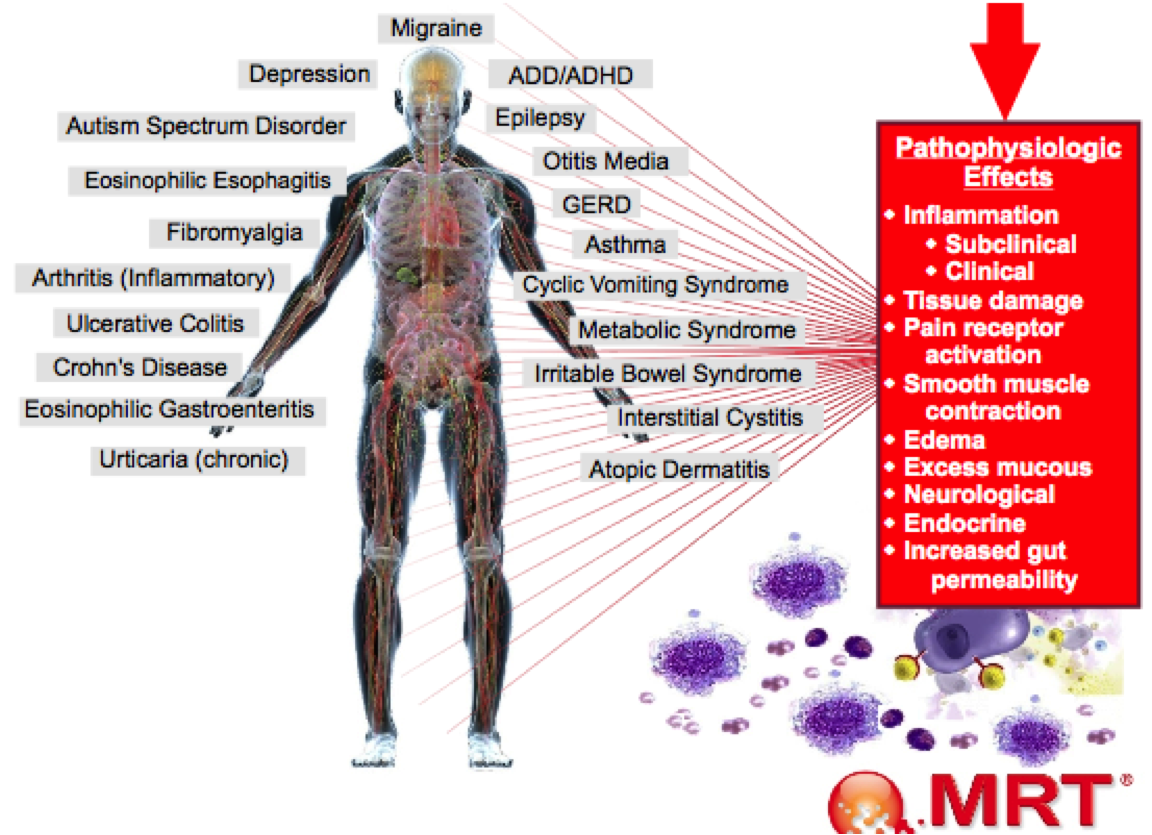
Conditions and Symptoms Related to Gut Problem
Most people assume that they have to have a digestive complaint before they pay attention to their gut. However, headache, migraines, allergies, food sensitivities, eczema, hives, psoriasis, depression, autism spectrum, diabetes, obesity, autoimmune conditions (like rheumatoid arthritis, type 1 diabetes, celiac, Crohns, colitis, MS), brain fog, anxiety, chronic fatigue, fibromyalgia, asthma, chronic sinusitis, and muscle and joint point are all related to the gut.
You don’t have to have gut symptoms to have leaky gut.
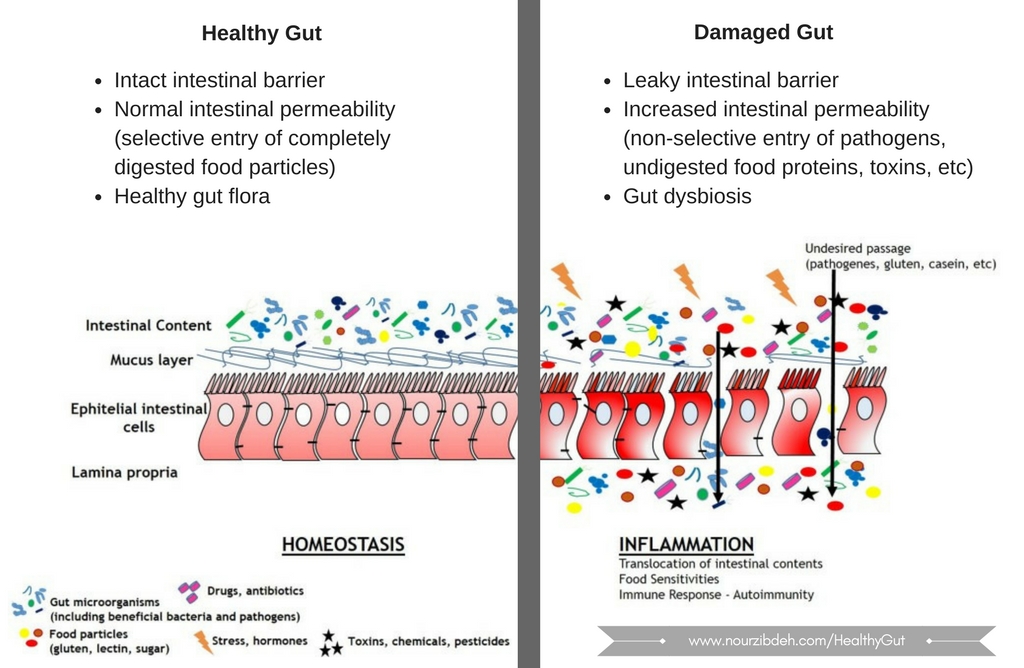
What Does it Mean to Have a Damaged or Inflamed Gut?
Gut damage or inflammation can mean that an one or both of these imbalances are occurring:
Gut Dysbiosis
This means an imbalance in gut flora, with reduced variety or number of healthy microbes or an overgrowth of bad microbes, or all of the above. Pathogenic gut microbe (like unhealthy bacteria, yeast, or parasites) do not support gut functions. They ferment food particles and cause gas, bloating, diarrhea, or constipation and produce toxins that inflame the gut further. If combined with leaky gut, toxins and by-products of microbes enter the body, causing headaches, brain fog, fatigue, joint pain, and more.
Leaky Gut
In leaky gut, or increased intestinal permeability, foreign particles like undigested food proteins, chemicals, toxins, microbes, and anything that should stay outside enter the body. The gut is leaking all these problem particles inside! In the intestine, 70-80% of the immune cells are waiting to attack these foreign substances. Activation of the immune system leads to inflammation that, if it goes unchecked for years, can cause autoimmune diseases. Leaky gut can also lead to food sensitivities.
What affects Gut Flora?
Your gut flora, the number of microbes and variety, depends on your age, gender, diet, geography, hygiene, stress and medication use. Babies born through vaginal delivery have better gut flora than babies born with C-sections. Babies who were breast-fed also have more friendly gut bacteria than bottle fed babies. Babies born to mothers with unhealthy gut flora are likely to develop gut-related issues and may be at higher risk for eczema, psoriasis, depression, overweight, and other conditions related to the gut.
What Damages the Gut?
1. Antibiotics
Antibiotics kill good and bad bacteria at the same time, reducing the diversity and number of the good healthy bacteria. Your body will try and rebuild some of it, but it won’t completely rebound. If you had to take multiple courses of antibiotics back-to-back, the effect will be cumulative. Without probiotics to replace healthy gut flora, the damage from antibiotics can be permanent. I always ask my patients if they were chronically sick babies or had to take too many antibiotics for chronic ear or sinus or other infections.
Antibiotics also kill acid-producing bacteria. While your body benefits from an overall alkaline pH, the stomach and intestine need to be acidic to prevent an overgrowth of candida (yeast). Chronic yeast infections are common in people with chronic antibiotic use. I even have patients who report a yeast infection every time they take an antibiotic course. It’s vicious cycle!
2. Non-steroid Anti-Inflammatory Drugs (NSAIDs)
Non-steroid anti-inflammatory drugs (NSAIDs), such as aspirin and ibuprofen, work by reducing the secretion of inflammatory prostaglandins. However, these prostaglandins have a protective effect in the gut, and lower levels of prostaglandins make the gut more vulnerable to injury.
Long-term use of NSAIDs will inflame the gut lining, increase intestinal permeability, change the composition of the gut flora, induce gluten sensitivity, causing more serious problems with long-term use. Better alternatives of NSAIDs include fish oil supplements and curcmin. I recommend high quality and potent products that are also available through my online supplement store (click on anti-inflammatory support). And the best approach would be to address the cause of inflammation, which can be nutrient deficiencies, gluten, food sensitivities, sugar, or processed foods.
3. Antacids
Stomach acidity is the first line of defense against the overgrowth of pathogens. Over-the-counter and prescription medications that lower the acidity of the stomach are detrimental to ghe gut because the encourage microbes to flourish. This includes proton pump inhibitors (PPIs) like Prilosec and Prozac and H2 blockers like Zantac or Pepcid. Popping too many Tums tablets or taking too much baking soda in an attempt to alkalize your body reduce stomach acidity.
Antiacid also disturb digestion. Stomach acid is necessary for digesting and absorbing amino acids, vitamin B12, and iron. Stomach acid stimulates the pancreas to secrete picolinic acid which binds to zinc, selenium, chromium, manganese, boron, molybdenum, and vanadium in the gut and facilitates their absorption. Without enough stomach acid, you’re not benefits from the good nutrients in the good healthy foods you worked hard to put on your plate.
4. Birth Control Pills
Birth control pills don’t directly affect gut bacteria like antibiotics. However, oral contraceptives promote estrogen dominance, which encourages candida (yeast) overgrowth. Oral contraceptives have been found to double the risk of yeast infections.
5. High Sugar Low Fiber Diet
Pathogenic bacteria and yeast feed on processed and refined sugar. Good bacteria and yeast feed on fiber from vegetables, fruit, tubers (like sweet potato), legumes, and unprocessed grains. Your gut will be populated with whichever group has more food. It’s that simple.
When good healthy bacteria ferment fiber, they produce short-chain fatty acids, like like butyrate, acetate, and propionate. These short-chain fatty acids nourish the cells that line the intestine, maintaining their health, integrity, and a strong healthy gut barrier. A diet that lacks natural food fiber eventually leads to gut dysbiosis and leaky gut.
6. Gluten (and sometimes all grains and legumes)
Gluten promotes the secretion of a protein call zonulin from the intestinal cells (study). Zonulin causes the tight junctions between cells to open up, making the gut permeable or leaky. While we all produce zonulin, the intensity and duration of its effect, widening of the tight junctions, vary from one person to another. Measuring zonulin is one of the ways to assess the presence and severity of leaky gut.

When your intestinal lining is permeable, undigested food particles, food chemicals and toxins, and microbial toxins enter from the gut through the intestine into the blood stream. This triggers immune reactions, including food sensitivities and autoimmune diseases.
Most people assume that if they don’t have celiac disease, they should not be concerned about removing gluten from their diet. However, that’s not true. Celiac disease is an autoimmune disease where the body attacks the intestine cells in the presence of gluten. A 100% gluten-free diet is required to for the gut to heal properly. However, there are people who test negative for celiac disease, yet respond really well when they eliminate gluten. Their symptoms just disappear. One of the things that could explain this is zonulin release and the permeability of the gut.
Since we’re on the topic of gluten, keep a note of this. All grains and legumes can damage the gut because they contain lectins that can cause gut irritation. Lectins are plants natural weapons. They resist digestion and can cause inflammation, especially in excess. Many people overeat other grains when they switch to a gluten-free diet. And fear not! You can get fiber without grains or legumes. Vegetables, fruit, and tubers are excellent and gentle fiber sources.
7. Low Thyroid Function
Optimal thyroid function is necessary for optimal digestive function. Low thyroid function has been associated with low stomach acid, and I have already talked about the consequences of that. When your thyroid is slow, gut movement is slow, and you end up with constipation. Waste can get stuck in pouches in the gut, leading to inflammation, fermentation, and bacterial overgrowth.
With constipation, by-products, waste, excess hormones, and compounds that your liver detoxed are stuck in the body, leading to brain fog, fatigue, muscle and joint pain, anxiety, moodiness and more. All of these just make lead to more inflammation and physical and emotional stress (who likes to be backed up!), which worsen your overall health. Read my article about thyroid health.
8. Infections and Overgrowth (Bacterial, Yeast, or Others)
An overgrowth of any pathogen, or dysbiosis, causes inflammation, disturbs digestions, and leads to leaky gut. Some of the common gut infections include candida (yeast), h Pylori, and small intestinal bacterial overgrowth. Low fiber and high sugar diet, chronic antacid and NSAID use, and even chronic use of sucralose (Splenda) promote dysbiosis. An infection or overgrowth can lead to chronic stress, leaky gut, food sensitivities, and autoimmune diseases. Combined with leaky gut, the toxins of these microbes can now freely enter the body and cause a wide range of symptoms.
These symptoms can be traced to gut dysbiosis or infections:

- Diarrhea or constipation, or both
- Gas and bloating
- Stomach or intestinal cramps
- Feeling very full quickly after eating, even when eating small amount of food
- Excessive burping and belching
- Brain fog
- Chronic fatigue
- Muscle and joint pain
- Behavioral and emotional issues (including children)
- Skin issues like blemishes, rashes, hives
- Excessive nasal secretions and post-nasal drip
- Sugar cravings
Undetected and untreated infections are the root cause of many gut and none-gut problems. A functional nutrition approach to healing the gut must assess the possibility of an overgrowth and address properly through diet and anti-microbial herbs. It’s not enough to quit sugar. That will only quiet the microbe and put it into hibernation. But once you start introducing sugars, even natural fruit, the symptoms come back again. In my practice, I asses the risk of bacterial or yeast overgrowth though symtpoms and medical history, diet, and stool testing, and my functional nutrition approach include specific diet protocols, anti-microbial herbal supplements, as well as nutrients to support and heal the gut.
9. Chronic Stress
Stress is a very general term and can mean different things to different people. It’s a real or perceived threat where you body feels the need to response to maintain stability and survival. Stress can be acute or chronic. It can be physical (injury, infection, gut dysbiosis, inflammatory diet, sleep deprivation, etc) or mental and emotional (work, relationships, finances, long commutes, etc).
How is stress related to the gut? The brain and the gut are connected through what is known as the brain-gut axis. What happens in the gut affects the brain, and that’s how dysbiosis can cause behavioral and emotional issues in adults and children. And the opposite is just as true. Stress disturbs normal gut function. It slows down digestion and absorption, lowers enzyme production, and reduces blood flow to the intestine. It increases intestinal permeability (leaky gut) and reduces your body’s ability to repair and regenerate new healthy intestinal cells. It can also cause dysbiosis, leading to leaky gut.
While acute stress subsides, allowing your body to return to normal function, chronic stresses, never go away. They are far more damaging because the body doesn’t get a chance to heal and recover. Chronic stress can lead to inflammatory bowel disease (IBD), irritable bowel syndrome (IBS), ulcers, food sensitivities, and gastroesophageal reflux disease (GERD).
How do I Heal my Gut?
As you can see, there are many things that can cause gut inflammation, dysbiosis, and permeability. You must address ALL pieces of the puzzle. It can take 3 to 6 months, and even a year or two for your gut to complete heal. But don’t be discouraged or overwhelmed. I starting seeing results with my patients in as short as 2 weeks.
Healing the gut begins with a proper assessment of medical history, diet, infections, lifestyle, medication use, travel history (and exposure to pathogens), and previous dietary and medication treatments to solve the problem. Since gut problems can be summed into dysbiosis and leaky gut, the nutrition therapies I use will support one or both of these.
Some of the tools and recommendations I use include:
- Gluten-free diet
- Grain, legume, and dairy-free diet (close to Paleo)
- Probiotics and fermented foods
- Bone broth
- Digestive enzymes
- Therapeutic diets like low FODMAPs and SCD
- Low sugar
- Food sensitivities testing and program
- Stool testing and anti-microbial protocols (SIBO, candida, h Pylori, and others)
- Functional foods and supplements for the gut, including glycine, glutamine, zinc, aloe, licorice and others
- Stress management
You can’t follow all of them at the same time. Based on a proper assessment and my clinical experience, I pull the right tool from the box and help you implement it. From experience, the best results have been when I combined few of these tools, usually staggered, to help my patients achieve complete healing.
What eventually matters the most is your ability to follow the diet, supplement, or lifestyle protocol. That’s how I can help. I combine my functional nutrition background with my skills and tips for meal planning and cooking to help you learn and practice these protocols. We check in regularly to make sure healing is progressing. And I support and cheer you as you push through the challenges and barriers. My commitment to you is to not stop looking for answers until we get to the root of the problem so you can finally live an energetic life, love your body and gut, and thrive.
Is Functional Nutrition approach right for you?
Attend my free training to learn more.
To help you answer this question, schedule a Strategy Consultation so we can map out your path to calming your immune system and restoring your health so you eliminate your symptoms and thrive.
Before working with Nour, I experienced intestinal pain off and on for for 54 years with minimal success on medications. I have benefited 100% from Nour’s program as I am now pain free!
– L.G.
A lot of time and money was wasted on foods that I thought would help my digestive struggles [diarrhea, bloating, hunger], but in fact I was making it worse. The main benefit is getting a handle on what negatively affects my digestive symptom. Doing a total 180 to my eating habits has been pretty amazing.
– J.V.


